Allergic Reactions: What to Look For and Do For Babies and Kids
An important reminder:
This post and anything on this website is for educational purposes only. It should not be used as medical advice or in place of or to delay seeking medical attention. Every child is different and has different needs. Your child’s provider can help you figure out the best management plan for your specific situation.
Let me start with something I want every parent to hear before anything else: most kids will never have a severe allergic reaction. Only about 8% of children in the United States have a food allergy.
Knowing that statistic doesn't make it any less terrifying when it's your child. And being prepared is not the same thing as being scared.
My daughter is one of the 8%.. I'm a pediatric nurse practitioner with over 13 years of experience — including time in the pediatric ICU. I have taken care of children in their worst moments, and still felt the fear when it was my own baby having a reaction. SO I GET IT!!!
That experience is a big part of why I'm writing this. Because I want every parent, grandparent, babysitter, and teacher to know what to look for and what to do — not from a place of fear, but from a place of real confidence. While also reminding you that while social media and the internet make it seem very common (especially in the setting of starting solids), it truly isn’t as common as we’re led to believe. Let's get into it.
Why you’ve started hearing “early introduction”
An allergic reaction happens when the immune system misidentifies a normally harmless substance as a threat. Most common include
food protein
an insect sting
medication
Materials or chemicals (i.e. latex)
as a threat.
The immune system launces a defense response and that is what produces the symptoms.
Reactions can range from very mild — a few hives, an itchy mouth — all the way to anaphylaxis, which is severe and life-threatening. Reactions can look different every single time, even in the same child. A reaction that was mild last time does not guarantee the next one will be mild too. This is one of the reasons having an action plan matters so much.
Signs of a Mild to Moderate Allergic Reaction
Mild symptoms include
an itchy or runny nose
sneezing
an itchy mouth or throat
a few isolated hives or mild skin itching
or mild nausea or a single episode of vomiting
What to do for a mild reaction: Remove your child from the exposure if you can. If it is food related, stop the food immediately. Watch your child closely, because reactions can progress. Call your pediatrician for guidance on next steps, including whether to give an antihistamine and which one to use.
A few things worth knowing here. Benadryl (diphenhydramine) causes significant drowsiness in babies and young children, which makes it genuinely harder to monitor how they're doing. Many pediatricians will actually prefer non-sedating antihistamines like cetirizine (Zyrtec) for mild reactions. Ask your child's doctor ahead of time what they recommend keeping on hand.
Really important:antihistamines cannot treat anaphylaxis. They can help with mild symptoms, but if a reaction is progressing or involves more than one symptom at the same time, you need epinephrine — not Benadryl. More on that below.
Signs of Severe Allergic Reaction (Anaphylaxis)
Anaphylaxis is a severe allergic reaction that affects breathing and/or circulation. It is a medical emergency, and it requires immediate action.
About 1 in 100 school-age children have a history of anaphylaxis — which means even if your child has never had a reaction, someone in their world likely has. This is worth knowing regardless of whether your child has a diagnosed allergy.
Signs of anaphylaxis — call 911 immediately:
Difficulty breathing, wheezing, or a repetitive cough.
Swelling of the face, lips, or tongue.
Widespread hives or a rash across the body (not just a few spots around the mouth).
Pale, bluish, or ashen skin.
Repetitive vomiting.
Sudden limpness, confusion, or loss of alertness.
A hoarse voice or a cry that sounds different than normal.
In babies specifically, anaphylaxis can look a little different. Watch for inconsolable crying that comes on suddenly, extreme drowsiness or unusual limpness, excessive drooling, or a baby pulling at their tongue or ear. Babies cannot tell you what they're feeling — which is what makes this age group particularly tricky to read. If something feels off, trust your gut and act.
If your child has a known allergy and has been prescribed an Epinepherine auto-injector, follow your provider’s Emergency Action Plan, adminster the epinepherine, and then call 911.
If your Child has a known Allergy…
Have a written Food Allergy and Anaphylaxis Emergency Action Plan. The AAP has a free downloadable plan at HealthyChildren.org that your child's doctor can complete with you. Print it. Share it with school, daycare, grandparents, and babysitters — everyone who spends time with your child needs to know it exists and know where to find it.
Keep epinephrine everywhere your child is. Home. School. Diaper bag. Car. This is non-negotiable. And make sure every person who cares for your child knows not just that it exists, but how to actually administer it.
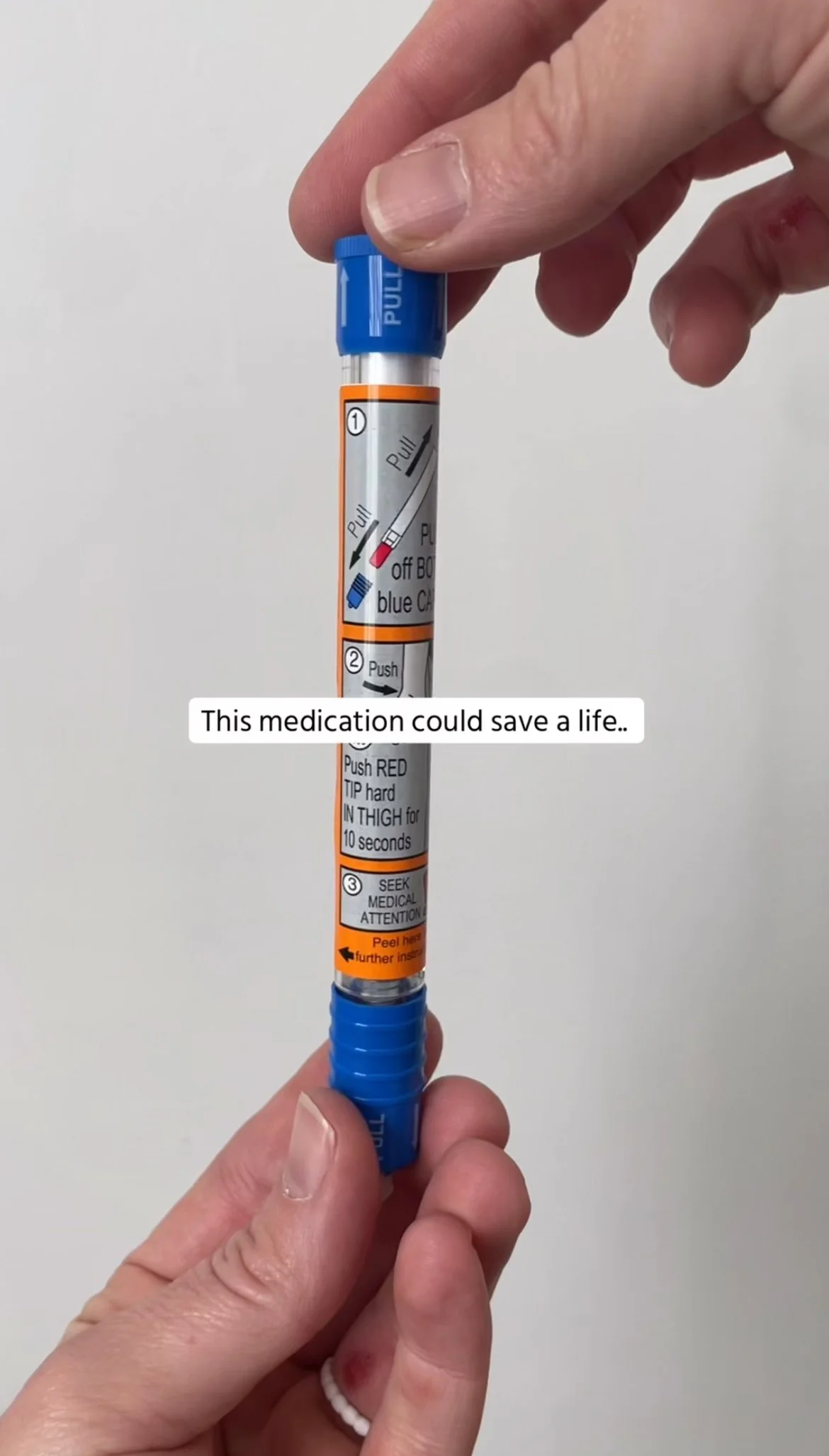
Know how to use their emergency medication (if it is an Epinepherine auto-injector, watch this video)
Consider a medical alert bracelet for children with a history of anaphylaxis. It gives first responders critical information immediately, even if you're not there.
Pro Tip
And here is something important to understand: a reaction doesn't always happen on the first exposure. The immune system is still learning during those early months. Most reactions happen on subsequent exposures — not always the first one. Just noting as a reminder that just because a reaction was mild this time, does not mean it will be next time.
Want to Feel Truly Prepared for a Pediatric Emergency?
Knowing the signs of an allergic reaction is a huge step. But real confidence comes from knowing what to do — including what to do if your child stops breathing, is choking, or is having a true anaphylactic reaction in front of you.
Our Baby + Child CPR, Choking, and First Aid class is built for exactly this. It's a hands-on training for parents, grandparents, and caregivers who want to feel genuinely ready — not just informed. We cover infant and child CPR, choking response, allergic reactions, fevers, bleeding, burns, head injuries, and so much more. Available as in-person community sessions, private sessions, and private virtual sessions.
Find your class and book your spot here.
And before you head out — grab our free guides for all of your first aid needs!
Your go-to resource for what to keep on hand to confidently care for your baby, child, and whole family through sick days, emergencies, and every day care!
Just want to stay in the loop: Join the Bite Sized Bits Newsletter below for practical pediatric tips delivered to your inbox — no overwhelm, just the things that actually matter.
Hi, I'm Cierra — a pediatric nurse practitioner, mom of three, and the founder of Bite Sized Peds. I help families feel genuinely confident in caring for their babies and kids, from first bites to first aid and everything in between.
-
Medical/General: The content, information, opinions, and suggestions listed here have been created with typically developing children and babies in mind. The information here is generalized for a broad audience. The information here should by no means be used as a substitute for medical advice or for any circumstance be used in place of emergency services. Your child is an individual and may have needs or considerations beyond generally accepted practices. If your child has underlying medical or developmental differences, including but not limited to prematurity, developmental delay, sensory processing differences, gastrointestinal differences, cardiopulmonary disease processes, or neurological differences, we strongly recommend you discuss your child's plan with the child's doctor, health care provider. By accessing this site and the information in it, you acknowledge and agree that you are accepting responsibility for your child’s health and well-being. By using and accepting the information on this site, the author (Cierra Crowley) is not responsible for any adverse effects or consequences resulting from the use of any suggestions discussed. It is important to talk to your child’s pediatrician or medical provider to start anything new or make any changes.
Affiliation: this page contains affiliate links from which I can earn small commissions (at no additional cost to you).
-
American Academy of Pediatrics. (2019). Guidance on introducing peanut-containing foods to infants to prevent peanut allergy. HealthyChildren.org. https://www.healthychildren.org/English/ages-stages/baby/feeding-nutrition/Pages/Peanut-Allergy-Prevention.aspx
American Academy of Pediatrics. (2019). Food allergies in children. HealthyChildren.org. https://www.healthychildren.org/English/healthy-living/nutrition/Pages/Food-Allergies-in-Children.aspx
Gupta, R. S., Springston, E. E., Warrier, M. R., Smith, B., Kumar, R., Pongracic, J., & Holl, J. L. (2011). The prevalence, severity, and distribution of childhood food allergy in the United States. Pediatrics, 128(1), e9–e17. https://doi.org/10.1542/peds.2011-0204
Sampson, H. A., Muñoz-Furlong, A., Campbell, R. L., Adkinson, N. F., Bock, S. A., Branum, A., ... & Decker, W. W. (2006). Second symposium on the definition and management of anaphylaxis: Summary report — Second National Institute of Allergy and Infectious Disease/Food Allergy and Anaphylaxis Network symposium. Journal of Allergy and Clinical Immunology, 117(2), 391–397. https://doi.org/10.1016/j.jaci.2005.12.1303
Simons, F. E. R., Ardusso, L. R. F., Bilò, M. B., El-Gamal, Y. M., Ledford, D. K., Ring, J., ... & Thong, B. Y. H. (2011). World Allergy Organization guidelines for the assessment and management of anaphylaxis. World Allergy Organization Journal, 4(2), 13–37. https://doi.org/10.1097/WOX.0b013e318211496c
Food Allergy Research & Education (FARE). (n.d.). About food allergies. https://www.foodallergy.org/resources/about-food-allergies
Gupta, R. S., Springston, E. E., Warrier, M. R., Smith, B., Kumar, R., Pongracic, J., & Holl, J. L. (2011). The prevalence, severity, and distribution of childhood food allergy in the United States. Pediatrics, 128(1), e9–e17. https://doi.org/10.1542/peds.2011-0204
Lack, G. (2008). Epidemiologic risks for food allergy. Journal of Allergy and Clinical Immunology, 121(6), 1331–1336. https://doi.org/10.1016/j.jaci.2008.04.032